Public HealthPublic PolicyConstitutional LawGovernment
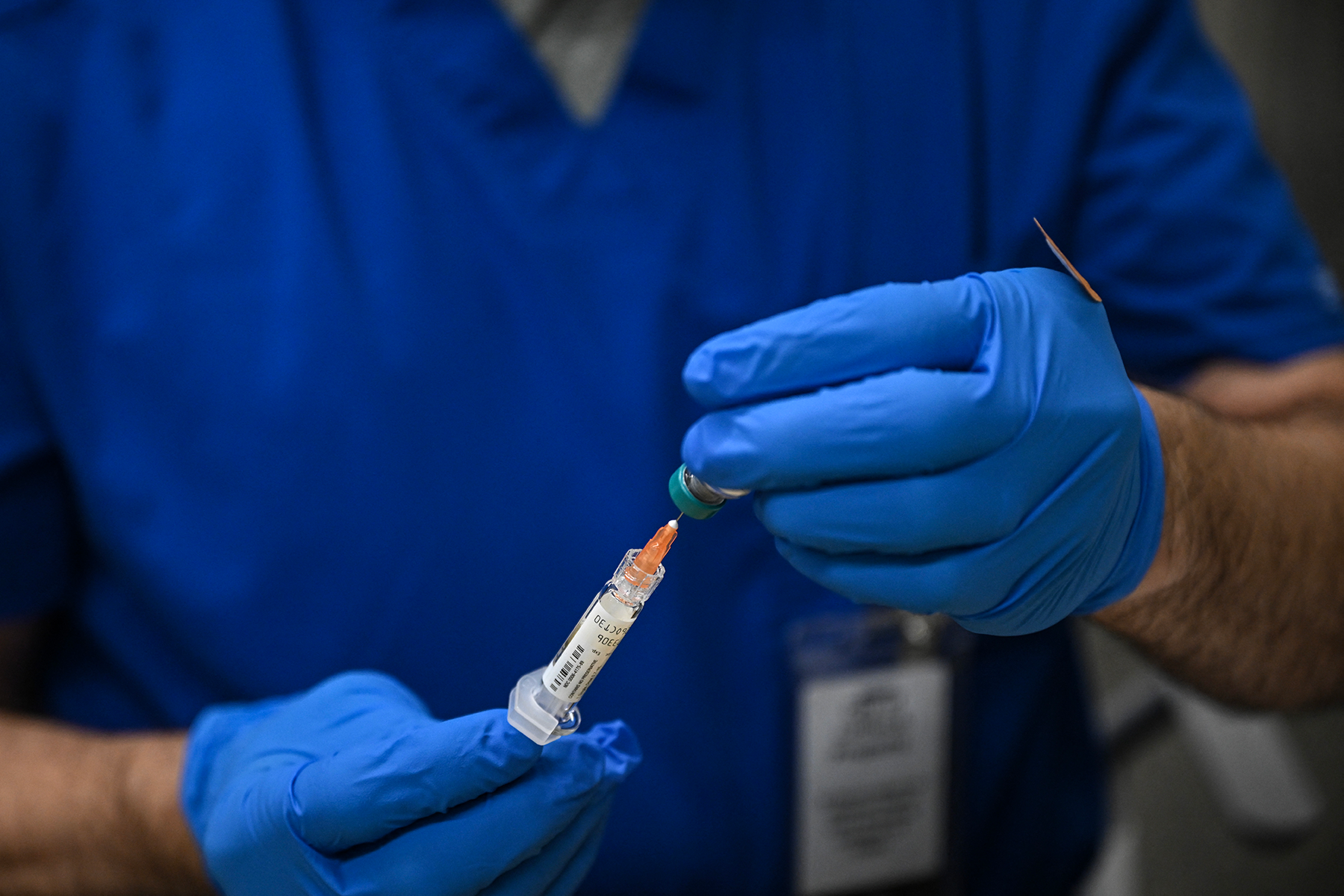
February 1, 2026FDA will now approve new drugs with one clinical trial instead of two, reversing a 60-year standard
The two-trial rule was created after thalidomide caused birth defects in 10,000 European children

Photo: Andrew Kelly / Reuters
On February 18, 2026, FDA Commissioner Marty Makary and Center for Biologics Evaluation and Research (CBER) Director Vinay Prasad co-authored a perspective article in the New England Journal of Medicine titled One Pivotal Trial, the New Default Option for FDA Approval. The article announced that FDA would default to requiring only one pivotal clinical trial plus confirmatory evidence for new drug approvals, replacing the longstanding expectation of two independent pivotal trials. Announcing regulatory policy through a journal article rather than through formal under the was itself unprecedented; Yale professor Joseph Ross told reporters FDA skipped the formal public comment process required for major regulatory changes.
The two-trial standard traces to the 1962 Kefauver-Harris Drug Amendments, passed by Congress after thalidomide caused severe birth defects including limb malformations in an estimated 10,000 children across Europe. The 1962 amendments required drugs to be proven effective through adequate and well-controlled investigations, plural. FDA interpreted this as requiring at least two independent controlled trials, ensuring a single favorable statistical result couldn't drive an approval by chance. Congress revisited the standard in the FDA Modernization Act of 1997, which explicitly authorized FDA to approve drugs based on one trial plus confirmatory evidence when sufficient. FDA never made one trial the default until Makary and Prasad's February 2026 article.
Clinical trials use a 95% confidence threshold, meaning researchers accept a 5% chance any result is a false positive. A second independent trial that must also succeed drops the probability of two false positives to 0.05 x 0.05 = 0.0025, or about 0.25%, a 20-fold reduction. Switching to one trial means accepting that up to 5% of approved drugs may appear effective by chance without actually working. Over hundreds of annual drug approvals, this could mean dozens of ineffective drugs reaching pharmacy shelves before post-market surveillance catches failures.
Under the new framework, the primary trial must be a well-designed randomized controlled trial demonstrating statistically significant efficacy on a clinically meaningful endpoint. Confirmatory evidence that can substitute for the second independent trial includes biomarker data, animal model evidence, data from related drugs in the same mechanistic class, real-world observational data from health records, and data from the same drug approved for a different condition. The FDA article did not specify what weight each type of evidence would carry or how agency reviewers would weigh a single positive trial against weak confirmatory evidence, leaving those determinations to case-by-case review per BioPharma Dive.
Richard Pazdur ran FDA's Office of Oncology Products for 26 years (1999-2025) and oversaw more cancer drug approvals than any individual in FDA history. He briefly took the role of acting CDER director at Commissioner Makary's urging before filing retirement paperwork in December 2025. STAT News reported he was handed a pre-written press release with a quote attributed to him about the single-trial policy and told to just agree to it, which he said he was undecided on and uncomfortable with. He told reporters: It's terrible to see 25 years of work dismantled. His departure, combined with CBER Director Peter Marks' forced resignation in March 2025 over RFK Jr.'s demands regarding the vaccine safety database, removed two of FDA's most experienced senior scientists within months of the administration taking office.
The policy change is expected to most significantly affect three drug categories: rare diseases, where small patient populations make two-trial designs difficult; cancer, where accelerated approval under surrogate endpoints is already common; and neurology and psychiatry, where clinical trial design is complex and the history of post-approval failures is extensive. The FDA separately issued a draft guidance on February 23, 2026 for a Plausible Mechanism Framework that allows ultra-rare disease drugs with no feasible clinical trial to seek approval based on biological mechanism alone. Critics of the single-trial change point to the 31 oncology drugs withdrawn after 2020 because their accelerated-approval confirmatory trials failed, and to Aduhelm, the Alzheimer's drug approved in 2021 over its advisory committee's 10-0 opposition that Biogen ultimately abandoned after it showed no meaningful clinical benefit.
Harvard Medical School professor Aaron Kesselheim, who directs the Program on Regulation, Therapeutics, and Law and resigned from an FDA advisory committee over the Aduhelm approval, warned that the FDA is already the fastest drug regulator in the world and that reviewing drugs on reduced evidence would require cutting corners. Yale's Joseph Ross raised the Administrative Procedure Act procedural argument, noting FDA has structured rulemaking procedures for new policies that were bypassed. A challenge under the APA could argue the announcement constitutes a legislative rule requiring notice-and-comment rulemaking rather than an informal guidance, which courts have sometimes invalidated when agencies skip the process.
The pharmaceutical industry spent a record $452 million lobbying in 2025, the largest single-year total ever recorded and up from $391 million in 2024. STAT News reported that three political firms with ties to Trump's inner circle collected nearly $11.7 million from pharmaceutical companies in 2025, compared to $2.2 million in 2024. Makary and Prasad argued in the NEJM article that lower capital costs for drug developers may remove a persistent justification for high drug prices. Critics noted cost savings from eliminating the second trial, estimated at $30 to $150 million per trial, accrue to pharmaceutical company shareholders rather than directly reducing what patients pay at the pharmacy.
The regulatory arc from 1937 to 2026 traces four distinct crises and four Congressional responses, each transferring risk in a different direction. The 1937 Elixir Sulfanilamide disaster — in which Massengill Company dissolved sulfa drug in diethylene glycol, killing 107 Americans, many of them children — produced the 1938 Federal Food, Drug, and Cosmetic Act requiring manufacturers to prove safety before marketing. The thalidomide near-miss (West Germany approved it in 1957; FDA reviewer Frances Kelsey refused from 1960 to 1962 despite repeated manufacturer pressure) produced the 1962 Kefauver-Harris Amendments requiring proof of efficacy. The AIDS crisis of the late 1980s — when patients were dying faster than FDA could review treatments — produced the 1992 Prescription Drug User Fee Act, creating an industry-funded review clock that has since grown to $1.43 billion annually in FY2026. The 2004 Vioxx withdrawal — Merck pulled the drug September 30, 2004, after its own APPROVe trial showed doubled cardiovascular risk; an estimated 88,000 Americans had heart attacks during the six years it was on the market — produced no structural reform. The 2026 single-trial default followed no crisis: it was driven by efficiency arguments and announced by journal article.
Black Americans bear a compounding disadvantage under the single-trial policy. A 2021 analysis published in Annals of Internal Medicine found Black Americans constituted 8.5% of interventional oncology trial participants from 2010 to 2021, despite representing 14.6% of the U.S. population — a participation-to-prevalence ratio of roughly 0.58. In multiple myeloma trials, where Black Americans develop the disease at approximately twice the rate of white Americans, median Black enrollment was just 4.5% of participants. When a drug is approved on a single trial with this enrollment pattern, Black patients receive less pre-approval evidence about how the drug works for them specifically. Post-market surveillance then adds a second gap: adverse event reporting through FDA's FAERS system skews toward patients with consistent healthcare access — historically higher-income and white patients — meaning harms in Black communities are less likely to surface quickly. Critics of the single-trial policy argue this double gap (thin pre-approval data plus slower post-market signal) falls hardest on patients who are already most underrepresented in the clinical trial system.
Related Topics
632 questions
Start the review